Case Sharing | Spinal Cord Stimulation for Rehabilitation of Incomplete Cervical Spinal Cord Injury
From: News Date: 2026-01-26 16:43Recently, the team led by Dr. Zhang Yongxiang, director of the Department of Rehabilitation Medicine at the Affiliated Hospital of Qingdao University, successfully performed spinal cord stimulation (SCS) on a patient suffering from intractable pain, limb movement disorders, limb numbness, and bowel and bladder dysfunction following a cervical spinal cord injury. The patient recovered well post-operatively, with significant pain relief, marked decrease in muscle tone, and improved lower limb muscle strength.
Case Summary
The patient, a 62-year-old male, fell while riding an electric scooter more than seven months ago, injuring his head and neck. Following the injury, he experienced limited mobility and pain in his limbs. He underwent a posterior cervical laminectomy with decompression and lateral mass screw fixation. Postoperatively, he received symptomatic treatment and rehabilitation, but continued to experience pain, limited limb mobility, numbness, urinary retention, and infrequent bowel movements. MRI revealed cervical spondylosis, herniated discs, and C3-C5 spinal stenosis.
Physical examination on admission: Generalized muscle atrophy; increased muscle tone in all four limbs, grade 2-3 on the modified Ashworth scale; left and right hip flexors strength grade 2+, left knee extensor strength grade 2, right knee extensor strength grade 2-, left ankle dorsiflexors and plantarflexors strength grade 2+, right ankle dorsiflexors and plantarflexors strength grade 2; decreased superficial sensation below T12 level on both the right and left sides, accompanied by pain and numbness, VAS score 8; knee and ankle reflexes (+++), bilateral Babinski sign (+).
Preliminary diagnosis: Chronic incomplete quadriplegia, motor dysfunction, cutaneous sensory disturbance, neurogenic bladder, neurogenic rectum, cervical spinal cord injury, post-cervical spine surgery, cervical disc herniation, type 2 diabetes mellitus.
Spinal cord stimulation (SCS)
After thorough examination and evaluation, and taking into account the wishes of the patient and his family, Dr. Zhang Yongxiang's team plans to perform spinal cord stimulation (SCS) surgery, primarily for the improvement of lower limb symptoms.
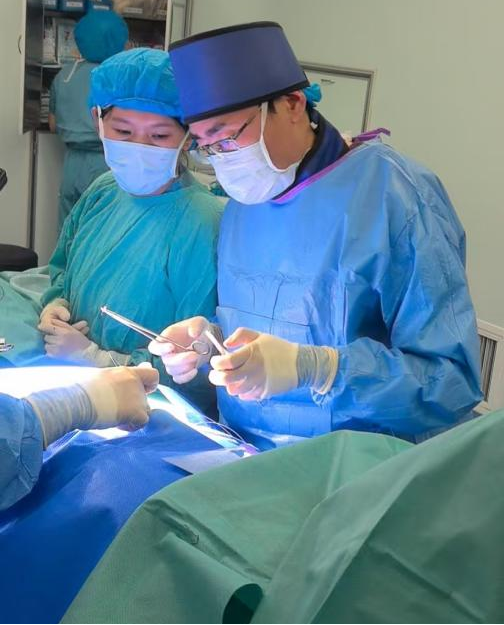
Two 8-contact needle electrodes were used for spinal cord stimulation and implanted in the T11-L1 segment. The location of the electrode implantation target was confirmed during the operation by combining imaging and the patient's subjective description.
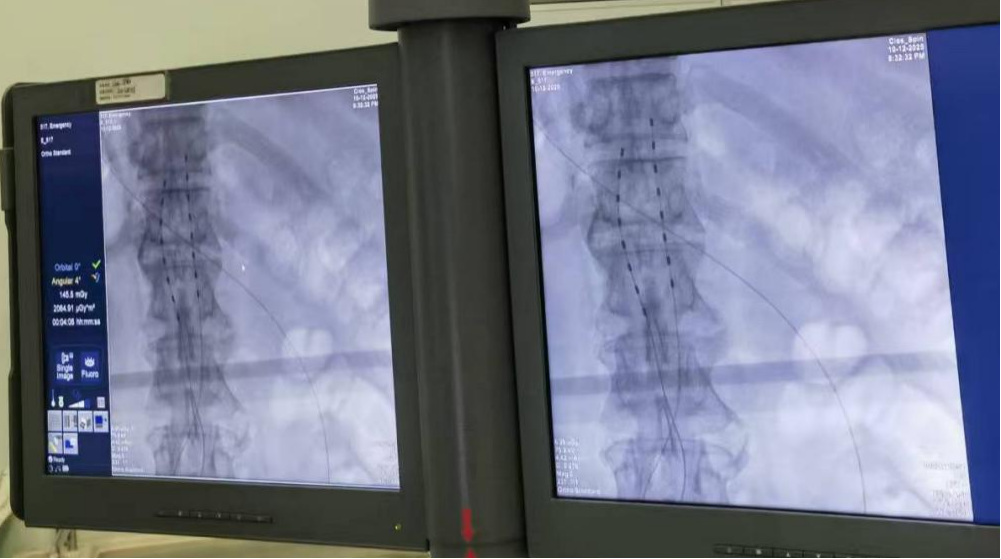
Intraoperative electrode imaging
After the stimulation was turned on postoperatively, the patient's pain was significantly relieved, and the VAS score dropped from 8 to 3; muscle tone decreased significantly, and the MAS score dropped from 2-3 to 1; the muscle strength of the lower limbs also improved, from 2 to 3-4, and the voluntary flexion and extension activities were significantly improved (the patient could not voluntarily flex and extend both legs when the stimulation was off, but could voluntarily flex and extend both legs after the stimulation was turned on).
Switch stimulation comparison video
Director's Comments
This case study, from a rehabilitation medicine perspective, demonstrates the unique value of spinal cord stimulation (SCS) as an adjunct neuromodulation technique in the comprehensive rehabilitation management of patients with incomplete cervical spinal cord injury. The efficacy observation in this case—significant pain relief, effective reduction in muscle tone (especially spasticity), and accompanying improvement in some muscle strength and motor control—provides a highly insightful clinical example for understanding and optimizing rehabilitation strategies for such patients.
I. Exploring the Mechanisms and Clinical Significance of Core Rehabilitation Benefits
Synergistic Regulation of Pain and Spasticity: The simultaneous improvement in pain and muscle tone in this case has profound clinical significance. Studies have shown that pain and spasticity often form a vicious cycle. SCS may inhibit pain transmission by stimulating the thick fibers of the posterior column of the spinal cord, based on the "gating theory." Simultaneously, its modulation effect may affect the excitability of α motor neurons and γ circuits in the anterior horn of the spinal cord, thereby breaking the "pain-spasticity" cycle. This not only alleviates symptoms but also clears key obstacles for subsequent active rehabilitation training, creating a valuable "therapeutic window."
The Rehabilitation Logic of Improved Motor Function: With pain and spasticity under control, the improved muscle strength and motor control exhibited by patients should be interpreted as a result of the combined effects of "neural function release" and "learned use." SCS may lower the "threshold" of motor output by providing a suitable neural electrical environment, allowing residual motor commands to more effectively control muscles, thus enabling patients to complete the task-oriented training designed by rehabilitation physicians with higher quality during treatment. This synergistic model of "neuromodulation-functional training" vividly embodies the modern concepts of precision and individualization in rehabilitation.
2. A New Paradigm of Team Collaboration from the Perspective of Rehabilitation Medicine
The success of this case highlights the core coordinating role of rehabilitation physicians in the entire management of SCS therapy. From the precise preoperative assessment of the patient's spasticity pattern, pain characteristics, and residual functional potential, to the postoperative dynamic adjustment of stimulation parameters based on patient responses (pain VAS score, Ashworth grade, muscle strength and function scales) and close integration with the training programs of physical therapists/occupational therapists, the rehabilitation team achieved comprehensive management from "implantation" to "integration." This transcends the realm of mere technical manipulation, entering a new phase of neurofunctional remodeling management oriented towards functional outcomes.
3. Cautious Optimism and Future Prospects
We must be keenly aware that the effectiveness of SCS in motor function recovery varies among individuals, and the maintenance of its long-term efficacy and optimal treatment parameter schemes still require further high-quality research validation. This case suggests that future research directions should include: utilizing rehabilitation assessment tools such as surface electromyography and three-dimensional motion analysis to quantitatively analyze the immediate and long-term impact of SCS on movement patterns and coordination; and exploring the optimal matching scheme between SCS parameters and different rehabilitation training techniques (such as motor relearning, forced movement therapy, and robot-assisted training).
Summary
This case powerfully demonstrates that spinal cord electrical stimulation can be a valuable "modulation tool" in the hands of rehabilitation physicians, rather than a "replacement therapy." By precisely intervening in the excitability of the spinal cord's neural networks, it "empowers" traditional rehabilitation training, helping patients better utilize their residual functions, thereby achieving breakthroughs in multiple dimensions such as pain management, spasticity control, and functional recovery. This motivates us to continue exploring the optimal path for combining neuromodulation techniques with evidence-based rehabilitation practices with a more integrated mindset and more refined solutions, creating more possibilities for the functional recovery of patients with spinal cord injuries.
Contact